July 06, 2020
First Nations Illicit Drug Deaths Rise during COVID-19 Pandemic
Data Release – COVID-19 Pandemic Sparks Surge in Overdose Deaths this Year
July 06, 2020
First Nations Illicit Drug Deaths Rise during COVID-19 Pandemic
Coast Salish Territory – The toll of the illicit drug toxicity crisis on BC First Nations individuals is rising again this year, erasing previous gains, according to data released today by the First Nations Health Authority (FNHA).
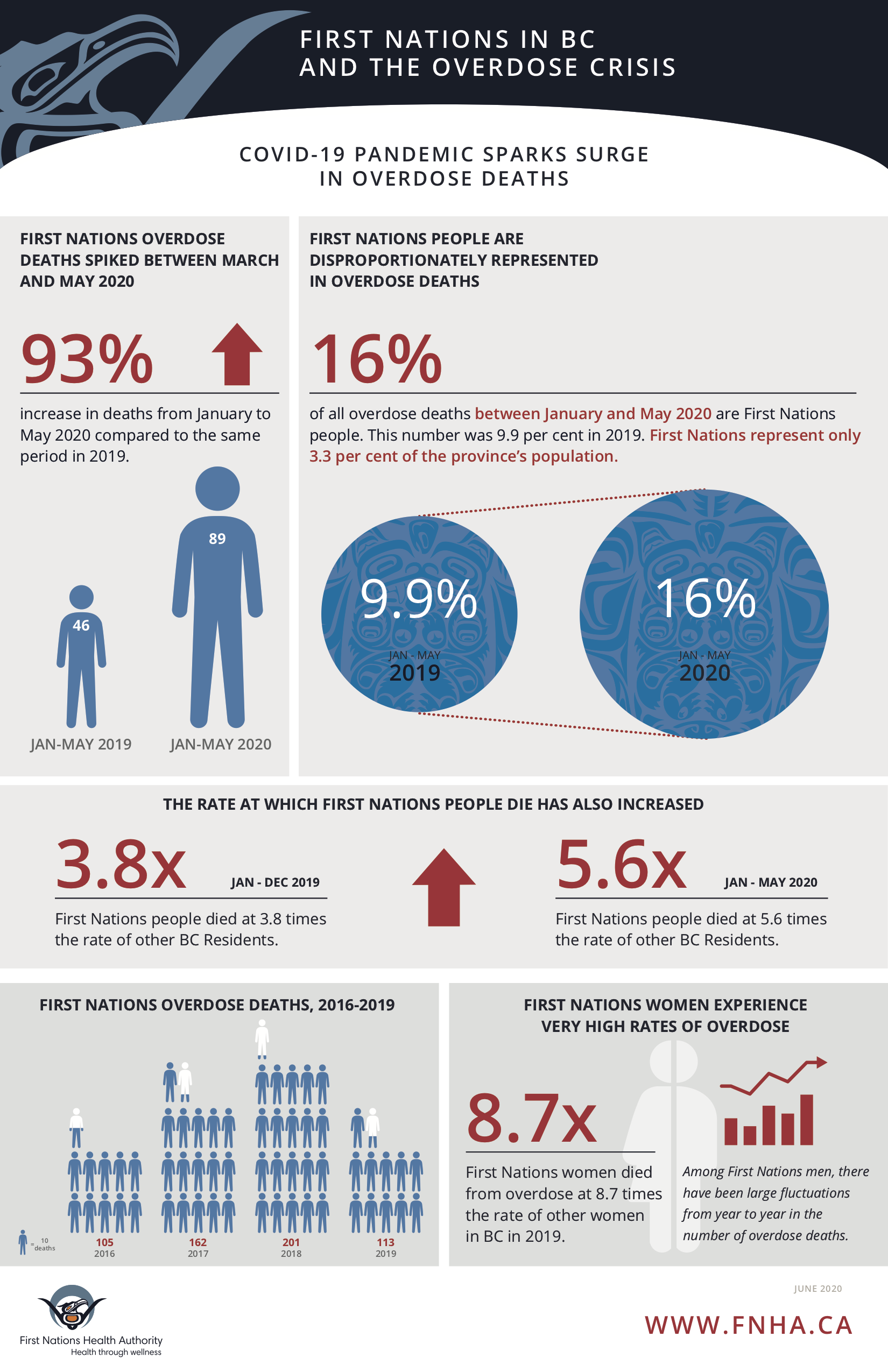
Suspected illicit drug toxicity deaths spiked between January and May this year. And during this period, 89 First Nations individuals lost their lives. This is a 93 per cent increase in deaths compared to the same period last year.
First Nations people represent 3.4 per cent of the province’s population yet accounted for a staggering 16 per cent of all overdose deaths in British Columbia from January to May of this year. So far this year, First Nations individuals have died at 5.6 times the rate of other BC residents, while in 2019 the ratio was 3.8.
COVID-19 safety measures have disrupted the drug supply, making the current supply more toxic.
Also, COVID-19 public health measures such as physical distancing and staying home may be having unintended negative consequences for people who use substances. People may be less likely to access harm reduction services and supports and may be using alone when they otherwise would not have.
The number of First Nations people dying from illicit drugs has increased significantly each year since 2016 when BC declared the public health emergency – except for in 2019, when there was a 44 per cent drop in overdose deaths. In 2019, 113 First Nations individuals died of an overdose; in 2018, the figure was 201 First Nations individuals.
There are many barriers to treatment for Indigenous people, including underlying systemic racism and experiences of stigma among people who consume alcohol and other substances. This points to a need for greater cultural safety and humility in health services.
Many First Nations people in BC are also less advantaged than other populations, creating vulnerabilities related to the social determinants of health like poverty and lack of housing, which are also predictors of substance use disorder and addiction.
Quotes:
“These data demonstrate that the opioid crisis continues to disproportionally affect vulnerable BC First Nations people. The concurrent COVID-19 pandemic is also creating challenges for those struggling with addiction,” said Charlene Belleau, Chair of the First Nations Health Council. “Properly resourced treatment centres and culturally safe harm reduction strategies will be critical moving forward. Now, more than ever, our people need this support.”
“This is truly devastating to all of us. We mourn deeply with each and every family for those we have lost to this terrible crisis.” said Judy Darcy, Minister of Mental Health and Addictions. “Indigenous Peoples are over-represented in this crisis and we are committed to working together with First Nations communities and leaders to create mental health and addictions services that are culturally safe and community led so that more families don’t have to keep experiencing these unimaginable and preventable losses of the people we hold close in our lives.”
“It is devastating for our families and communities to lose loved ones to the combined opioid and COVID-19 crises,” said Colleen Erickson, Chair of FNHA’s Board. “This forces us to renew our efforts to connect with and support those who are now more vulnerable than ever.”
“Our partners are going to be the key to finding effective and innovative solutions to this challenge,” said Richard Jock, FNHA’s Interim Chief Executive Officer.
“These numbers are telling us we need to do more to support our people with harm reduction and access to safe supply because the COVID-19 pandemic is increasing vulnerability to poisoned drugs,” said Dr. Shannon McDonald, Acting Chief Medical Officer of the First Nations Health Authority.
“In many cases, underlying chronic, severe trauma is related to substance use and during these dual public health emergencies it becomes even more important to increase mental health and wellness supports for BC First Nations people,” said Dr. Nel Wieman, FNHA’s Acting Deputy Chief Medical Officer.
“The illicit drug toxicity crisis in B.C. has resulted in a heartbreaking number of deaths in communities across British Columbia and, as we see from the Coroners Service data reported to the First Nations Health Authority, has impacted Indigenous people at an even more tragic rate,” said Lisa Lapointe, BC’s Chief Coroner. “We know the drug supply in British Columbia is dangerously toxic; the data being shared today represents a clear signal that all levels of government must urgently improve access to safer supply and to evidence-based, culturally safe, supports and services for those experiencing problematic substance use.”
“The increase in overdose deaths amongst Indigenous people in B.C. is deeply concerning. The COVID-19 pandemic is forcing all of us to stay farther apart from others, isolating people and adding to what is already an immense challenge, said Dr. Bonnie Henry, B.C.’s provincial health officer. “We need people living with substance use and addiction to know that there are still supports in place to keep people safe and prevent overdoses.”
BACKGROUNDER: FNHA ACTIONS TAKEN TO PREVENT OVERDOSE IN 2019-2020
To find out more about the First Nations Health Authority, visit: www.fnha.ca